5 min read
Caregiver Checklist: How To Reduce Hospital Readmission
By: Linda Ward on July 13, 2021 at 5:00 PM

In an ideal world, everything would always be seamless. Caregivers and family members would have all the tools in their belt to prevent mishaps from happening. Urgent hospital visits would be a thing of the past and all parties would be on the same page when it comes to long term care.
Unless you are a superhero, or have cared for somebody in the past, the likelihood that the scenario mentioned above becomes a reality is slim. The truth is discharge planning, especially when you’re still learning how to be a caregiver, can be a headache. Luckily, there are several tools and resources out there to help during this transition.
This blog will cover the topic of rehospitalization and the steps you can take to prepare for your loved ones return home and how to lower the risk of being readmitted.

The Key To A Successful Recovery Is Planning
Patients, caregivers, and healthcare providers have a vital role in determining what happens after a patient is discharged. Doctors are responsible for handling all medical assessments, and it is the caregiver’s job to represent the patient’s best interests. This is where discharge planning comes in handy.
Medicare defines discharge planning as the care a person needs after they leave the hospital, with the goal of preventing future readmissions. These plans are designed to facilitate a smooth transition from hospital to home or care facility. Even though a doctor makes the final approval of discharge from the hospital, discharge planning is often a team effort. This team usually consists of:
- Nurses will help you understand medication doses, pain management, and how to prevent the wound from becoming infected.
- Social Workers will help you create a discharge plan and discuss different long-term care options that your loved one might benefit from.
- Case Managers will do an assessment of your loved ones time at the hospital and work with the social worker to find referrals for long-term care.
Members of the medical care team will have information and resources about the care your loved one will need after leaving the hospital, but they are not experts on everything. That is where you, as a caregiver, can step in and be a vital member of the team. Think of any mental, emotional, or environmental limitations you and the person you are caring for might experience. Talk to the care team about those concerns during the discharge planning process so that they can be addressed ahead of time.
Caregiving limitations could be things like a job, childcare or other day to day responsibilities. It is important to look at all possible limitations and do check-ins with yourself. After all, the transition from relative to caregiver can be overwhelming. Take a moment to ask yourself “how am I feeling today?” and be honest with your emotions. During the discharge process you can ask the case manager or social worker for information about caregiver support groups. As well, ask if they can provide resources about caregiver burnout.
How Can I Prepare For My Loved One’s Return Home?
Studies have shown that on average approximately 11%-23% of Medicare patients over the age of 65 are readmitted to the hospital after 30 days. Readmission is not only stressful for someone that was recently discharged, but it puts stress on the body and immune system as well.
Readmission tends to happen because of mishaps related to medication management, slips or falls in the home, and poor wound care or hygiene. Often times, these reasons can easily be avoided with planning ahead, and reduce the chance of being readmitted to the hospital.
Preparing a Safe Home. New medications or tired muscles can make your loved one feel weak and dizzy. Before your loved one is discharged, consider taking a walk around the home and finding any potential tripping hazards. These could be things like rugs, steep or slippery stairs, dark walkways and hallways. You may also want to purchase items to help them stay steady, such as handrails for long hallways or a shower seat to make bathing easier and more accessible.

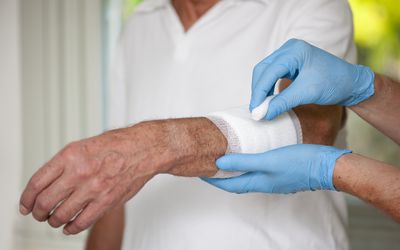
Wound Care. As the body ages, wounds take longer to heal and the risk of infection increases. Inefficient hygiene or wound care is another reason for why older patients are often readmitted to the hospital. Consider asking your loved one’s medical care team what signs of infection you should look out for, how often wounds need to be cared for, and if or how you should be changing the bandages. You can also keep a record of the healing progress and share that information during a follow up appointment.
What Happens Next?
If this was a perfect world, caregiving would be a breeze — but it’s not. If this you are reading this blog article and feeling overwhelmed by all of this information and the idea of discharge planning, don’t be afraid to ask for help. The Gulfside Home Health team has numerous resources and qualified staff that can assist you with the discharge process. You can schedule a consultation today and speak with a team member about services that your loved one might benefit from after they leave the hospital.
To get in contact with a member of the Gulfside Home Health team, call us anytime at 800-817-9941 or visit gulfsidehomehealth.org.
Related Posts
How do I know when my loved one is ready for hospice?
Discussing hospice can be a beneficial option at any stage of a life-limiting illness. Patients as...
Hospice or Palliative: Understanding the Difference
Hospice Care
Hospice care is palliative by nature, meaning it provides comfort care. At the point...
Hospice Care is Growing Nationwide — and Florida is Leading the Way
For the first time since before the pandemic, more than half of Medicare patients at the end of...




